


Patients with rheumatoid arthritis (RA) have a higher risk of cardiovascular disease (CVD) compared to the general population, which leads to increased morbidity and mortality. Inflammation is the key in RA and CVD. Our study aimed to refine cardiovascular (CV) risk assessment in RA patients by using carotid intima-media thickness (cIMT) as a marker of subclinical atherosclerosis. We also explored whether proinflammatory cytokines represented by tumor necrosis factor-alpha (TNF-α) and high-sensitivity cardiac troponin I (hs-cTnI), a biomarker of myocardial injury, could be correlated in RA patients. The study included 80 RA patients and 80 control subjects. TNF-α and hs-cTnI levels were measured. Subclinical atherosclerosis was evaluated by cIMT by means of carotid ultrasound. Disease activity score 28 (DAS28) was used to evaluate disease activity. hs-cTnI and TNF-α serum levels were higher in RA patients compared to controls (p=0.001). There was a significant difference in the median of cIMT between cases and controls (median (IQR) 0.9 (0.2) for cases, 0.7 (0.1) for controls, (p=0.001). A significant correlation was found between the level of TNF-α and hs-cTnI (p=0.002). Also, there was a significant correlation between the cIMT level and TNF-α and hs-cTnI (p=0.003 and p=0.002, respectively). Significant correlation was found between cIMT, TNF-α, and hs-cTnI in relation to the DAS28 score (p < 0.001, p < 0.001, and p=0.001, respectively). In conclusion, patients with RA are more likely to develop subclinical atherosclerosis, as reflected in increased cIMT. Higher levels of hs-cTnI in RA patients may correlate with the presence of occult cardiovascular disease. TNF-α and hs-cTnI correlations can reveal the interplay between disease activity and CVD. Thus, inflammation must be the primary target of various therapeutic approaches.
Background: The treatment of patients with relapsed or refractory non-Hodgkin lymphoma remains challenging. The strategy for management of relapsed or refractory disease is to deliver salvage chemotherapy, followed by autologous stem-cell transplantation in responding patient. Such salvage therapies typically consist of cytotoxic agents that have not been used in first line therapy.
Aim of Study: In this study we are trying to study one of the salvage chemotherapy lines which is GDP regarding response rate, quality of life and toxicity.
Patients and Methods: Seventy patients diagnosed as refractory or relapsed NHL were included in the study; all patients received GDP for 4 to 6 cycles. Primary end point was to evaluate overall response to treatment; secondary end point was to evaluate quality of life and toxicity. An informed written consent was obtained from all the patients and approval of Research Ethics Committee of Assiut, Faculty of Medicine was obtained prior to the study.
Results: The overall response was 65% with complete response 25% and partial response 40%. Regarding quality of life it was noticed that 32.9% patients using GDP were improved, 40% were stable patients while significant deteri-oration occurred in 27.1%. Regarding toxicity profile, occur-rence of neutropenia was 50% with grade III-IV 15%, throm-bocytopenia 40% with grade IV-V 5%, anemia 60% with grade II-III 7%. Nausea 50% with grade III-IV 3%, vomiting 40% with grade III-IV 10%, diarrhea 34.3% with grade II-III 5%. Renal toxicity 31.4% with grade I-II 15%, neurological toxicity 40% grade I-II 10%. Hepatic toxicity 25.7% with grade I-II 20%.
Conclusion: GDP is effective as second line chemotherapy with good response rate, quality of life and a manageable range of toxicity
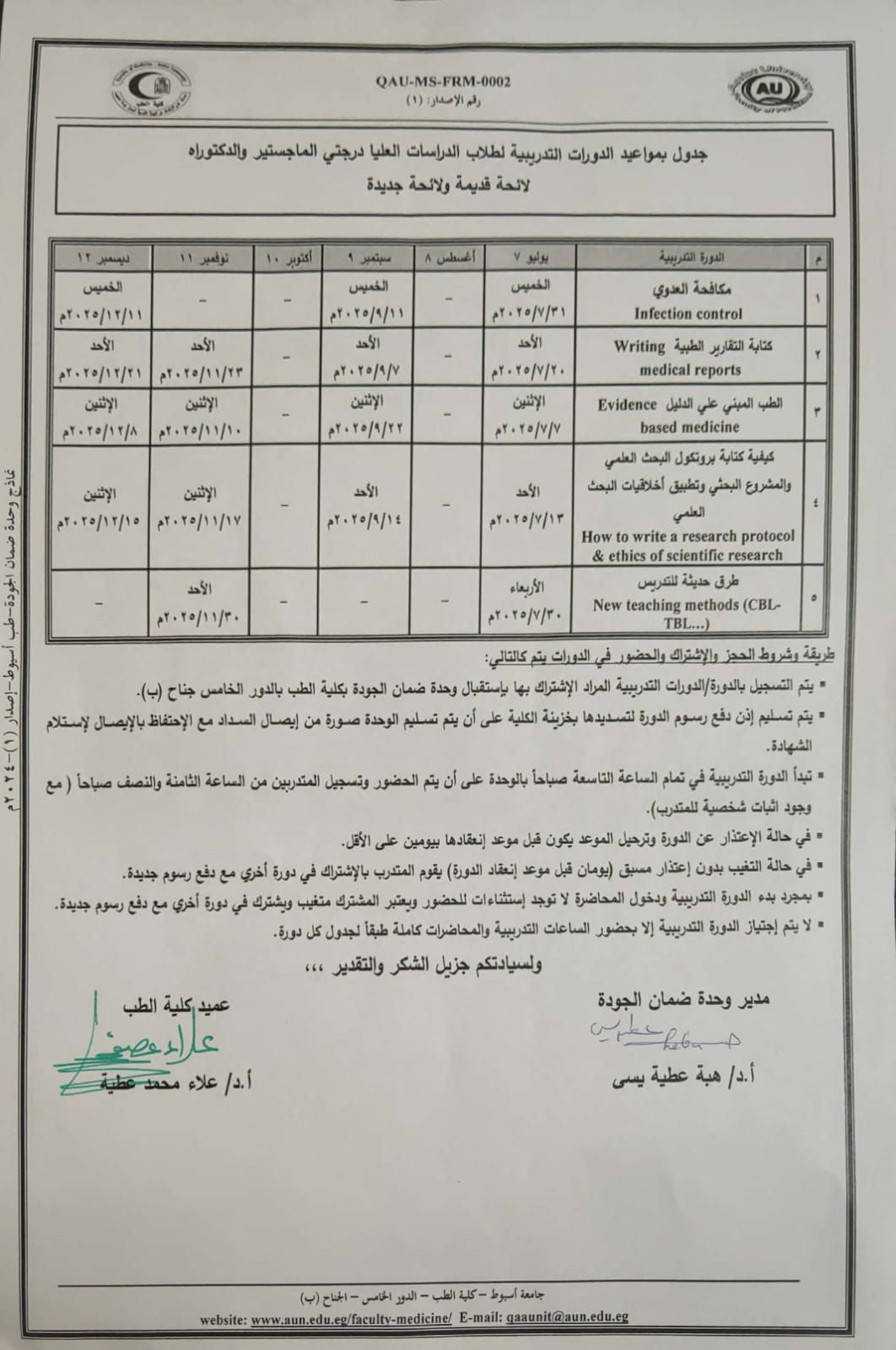
Training schedule for postgraduate students at the master's and doctoral levels. Old and new regulations.

Conditions for applying for scientific research funding for faculty members
Background: Type 2 diabetes mellitus (T2DM) is a long-term metabolic disease defined by reduced pancreatic β-cell function and impaired insulin action in peripheral tissues, which cause sustained irregularities in glucose homeostasis, mild inflammation. Objectives: Recent study aimed to detect levels of circANKRD36 in white blood cells of T2DM patients and examine their relationship with pro- inflammatory mediators (TNF-α and IL-6) in DN patients withT2DM and to evaluate the role of circANKRD36 in the initiation and development of DN. Methodology: Blood samples obtained from people with diabetes mellitus type 2 (69) cases and Control participants (23). Reverse transcription-quantitative polymerase chain reaction (RT-qPCR) was applied to evaluate levels of CircANKRD36. Levels of pro-inflammatory cytokines such as interleukin IL-6 via chemiluminescence and tumor necrosis factor (TNF)-α was determined via enzyme-linked immunosorbent assay (ELISA). Results: CircANKRD36 showed high expression levels in patients with T2DM and DN, contribute to the development of DN and it was superior to inflammatory markers in detection of early stages of DN. Conclusion: CircANKRD36 levels were markedly up-regulated in T2DM patients in comparison to control group (P=< 0.001).

