Announcement of the scientific symposium entitled “Applications of Artificial Intelligence in Digestive and Infectious Diseases”
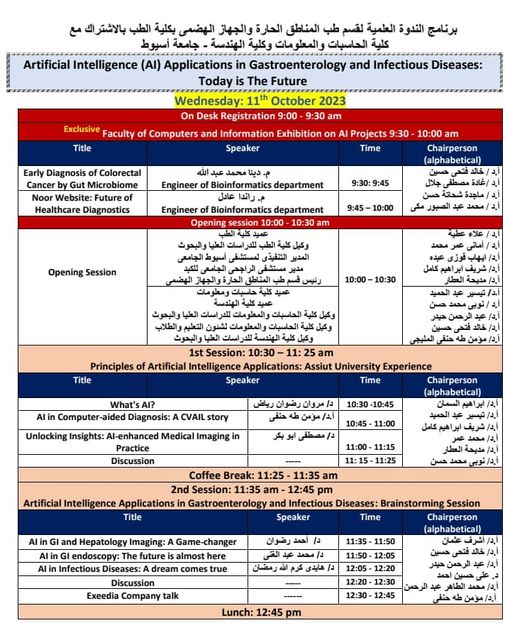
اعلان الندوة العلمية بعنوان " تطبيقات الذكاء الاصطناعي في أمراض الجهاز الهضمي والأمراض المعدية" تحت رعاية الدكتور أحمد المنشاوي -رئيس الجامعة الدكتور علاء عطية- عميد كلية الطب ورئيس مجلس إدارة المستشفيات الجامعية الدكتورة أماني عمر -وكيل الكلية لشئون الدراسات العليا والبحوث الدكتور إيهاب فوزي- المدير التنفيذي للمستشفيات الجامعية الدكتور شريف إبراهيم كامل- مدير مستشفى الراجحي. تأتي الندوة في إطار التعاون بين قسم طب المناطق الحارة والجهاز الهضمي بجامعة أسيوط وكلية الهندسة وكلية الحاسبات والمعلومات. بالتنسيق مع الدكتور نوبي محمد حسن -عميد كلية الهندسة الدكتورة تيسير حسن عبد الحميد- عميد كلية الحاسبات والمعلومات والدكتورة مديحة العطار- رئيس قسم طب المناطق الحارة والجهاز الهضمي. تستهدف الندوة التعرف على كيفية الاستعانة بالتكنولوجيا الحديثة للكشف المبكر عن أمراض الجهاز الهضمي لتجنب حدوث مضاعفات. يأتي اليوم بتنظيم من الدكتورة هايدي كرم الله رمضان، والدكتور أحمد رضوان رياض مقررا الندوة.
 Do you have any questions?
Do you have any questions? 


